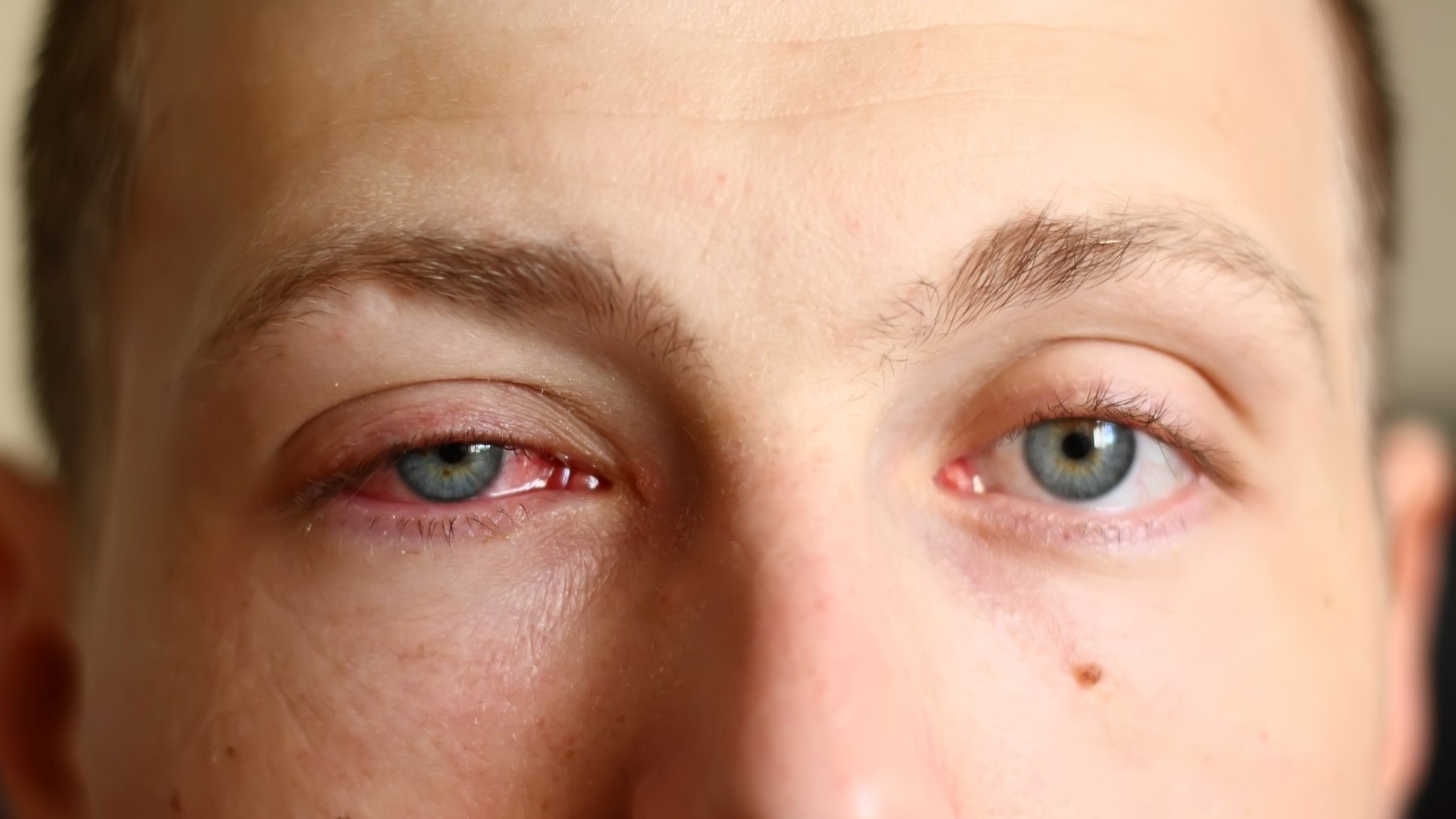
During the spring and summer months, patients frequently present to the pharmacy seeking professional advice for ocular disorders. One of the more common eye conditions pharmacists will be asked about during their career is conjunctivitis, more commonly referred to as “pink eye.”
Conjunctivitis is an umbrella term that refers to inflammation of the membrane covering the white of the eye and inside of the eyelids, known as the conjunctiva.1 There are three subtypes of conjunctivitis, with the classification depending on the cause: bacterial, allergic, and viral.

Bacterial Conjunctivitis
Acute bacterial conjunctivitis is characterized by copious purulent discharge, redness, and a foreign body sensation in the eye. Although it shares many overlapping symptoms with the other forms of conjunctivitis, the most distinctive features of bacterial conjunctivitis are bilateral matting of the eyes in the morning, and a lack of pruritis. 2
Although bacterial conjunctivitis is usually self-limiting in nature, the use of antibiotic eye drops may be considered to help expedite the resolution of symptoms and infection.3 Over-the-counter products such as polymyxin-bacitracin can be offered as treatment and typically are sufficient for most cases. In the event this is unavailable, or at the clinician’s discretion, prescription strength antibiotic eye drops or ointments can also be considered. 2
Viral Conjunctivitis
Most cases of conjunctivitis are caused by viruses.2 Some hallmark features include unilateral presentation, watery discharge, and itching. Since viral conjunctivitis is self-limiting in nature, treatment such as cold compresses and artificial tears may be recommended to provide symptomatic relief, however patients should be advised that antibiotic eye products have no benefit for viral infections. 3 Beyond providing options for symptomatic relief, pharmacists can reassure their patients that viral conjunctivitis typically resolves within 2 to 3 weeks on its own with a peak in severity 4 to 5 days after symptom onset.4
Allergic Conjunctivitis
Pharmacists are commonly consulted during allergy season by patients for ocular self-care remedies. Bilateral redness, itching and watery eyes, a history of allergies and symptoms that gradually disappear when the patient is no longer in proximity to the allergen are indicative of allergic conjunctivitis. These patients also typically present with non-ocular symptoms such as a stuffy or runny nose.
For mild cases, allergen avoidance, as well as the use of cold compresses and tear substitutes (which help dilute ocular allergens and prevent them from interacting with the ocular surface) may provide adequate relief. However, some patients may require stronger therapy, and may benefit from products containing an antihistamine such as levocabastine to help relieve itching and watery eyes. 3 Other treatment options for allergic conjunctivitis include mast-cell stabilizing agents such as sodium cromolyn and nedocromil, or eye drops containing olopatadine which has anti-inflammatory, mast cell stabilizing and antihistamine properties.5
Non-Pharmacological Measures
While allergic conjunctivitis is not contagious, viral and bacterial conjunctivitis can easily spread. Patients should be advised to remove contact lenses and avoid wearing them while infected, avoid rubbing their eyes, and to frequently wash their hands, particularly before and after administering medications to the affected eye(s).1
When to Refer Patients
There are situations where patients coming into the pharmacy for self-care options would be better served by scheduling a doctor’s appointment. If a patient has inflammation of the eye, vision is typically normal when the cause is conjunctivitis. Patients who present with “red flag” symptoms (e.g., eye pain, reduced visual acuity or altered vision, photophobia, headache with nausea, a fixed pupil, an opaque cornea, an inability to keep the eye open, and ciliary flush) or those who wear contact lenses should be referred to a specialist for further investigation to rule out more serious diagnoses. 3
Patients should also be referred to an ophthalmologist or optometrist if they have not seen significant improvement after 48 hours of treatment, or if their condition worsens following initiation of therapy.
References
- Protect Yourself from Pink Eye. (2021, November 12). Centers for Disease Control and Prevention. Retrieved July 18, 2022, from https://www.cdc.gov/conjunctivitis/
- Visscher, K. L. (2009, November 1). Evidence-based treatment of acute infective conjunctivitis. The College of Family Physicians of Canada. https://www.cfp.ca/content/55/11/1071
- Morrow, G. L. (1998, February 15). Conjunctivitis. Retrieved July 18, 2022, from https://www.aafp.org/pubs/afp/issues/1998/0215/p735
- Ryder EC, Benson S. Conjunctivitis. [Updated 2022 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541034/
- Uchio E. Treatment of allergic conjunctivitis with olopatadine hydrochloride eye drops. Clin Ophthalmol. 2008 Sep;2(3):525-31. doi: 10.2147/opth.s3294. PMID: 19668750; PMCID: PMC2694001.